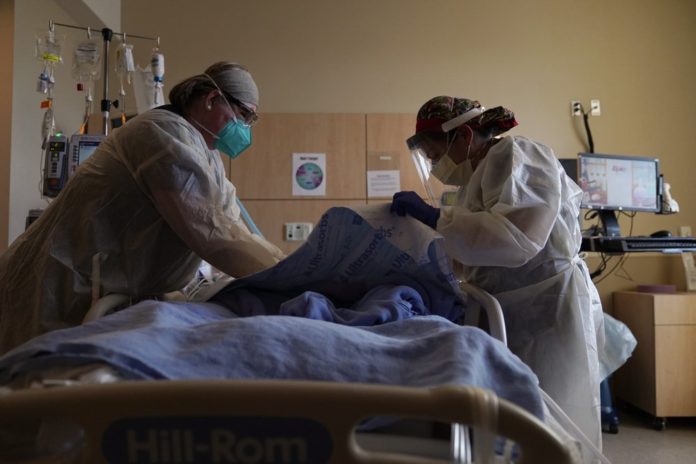
Hospital executives and public health authorities across Arizona pleaded Tuesday for people to get vaccinated and do everything possible to avoid spreading the coronavirus as they gird for another surge in cases that threatens once again to overwhelm the state’s health care system.
The numbers of coronavirus infections and hospital stays are trending up, as they did this time last year as families gathered for the holidays, culminating in a crushing demand at hospitals.
“Our messaging today is to ask for assistance. We need less COVID patients,” Dr. Marjorie Bessel, the chief medical officer at Banner Health, said during a news conference with the top doctors from the state’s major health care systems.
The physicians said vaccinations are the best way to preserve hospital beds. Vaccines keep most people from getting infected when exposed to the coronavirus, and even those vaccinated patients who do get sick are highly unlikely to be hospitalized or require intense levels of care.
They also urged people to skip Thanksgiving dinner if they’re not feeling well and to be tested promptly. Fast detection is necessary for treatment with monoclonal antibodies, which can keep COVID-19 infections from becoming critical.
People can comfortably go to holiday gatherings with a small group of vaccinated people but should avoid or at least wear a mask at larger gatherings where it’s unclear if others are vaccinated, the doctors said. They acknowledged that many people are tired of virus mitigation measures but said it’s critical that they continue taking steps to control the viral spread, including wearing masks.
The hospital overload is already crippling the Copper Queen Community Hospital in Bisbee, which this week closed its operating room to reassign those nurses to care for inpatient cases. That meant canceling 17 colonoscopies on Tuesday, said Dr. Edward Miller, chief medical officer at the 13-bed hospital.
Someone spent all day searching for a hospital to take a critical patient with congestive heart failure and in need of dialysis before finally transferring the person late Monday night, Miller said. The hospital, which lacks an intensive care unit, doesn’t normally care for critical patients.
“We are having problems down here,” Miller said.
Arizona hospitals are used to seeing a big influx of patients in the winter as respiratory viruses like the flu abound and the population swells with tourists and snowbirds, many of them elderly. Adding COVID-19 to the mix adds a significant strain.
Dr. Richard Carmona, a former U.S. surgeon general who is now Gov. Doug Ducey’s adviser on COVID-19, appealed to people to look beyond their sense of individualism and get vaccinated for the good of their family and community. But pressed repeatedly on whether Ducey is undermining public health messages by declining to wear a mask indoors himself, Carmona avoided criticizing the governor who hired him.
“I see some public officials wearing masks, and I applaud them for doing that,” Carmona said. “But we don’t have the authority to order anybody to do anything.”
Among the toughest challenges for hospitals has been staffing. Doctors, nurses, and respiratory therapists are exhausted after nearly two years of treating COVID-19 patients. And the competition for new hires and temporary help is fierce as infections rise throughout the country and the world.
“Just because we have ventilators available in our warehouse does not mean that we either have a place to send them or we have staff that is trained to support them,” Dr. Theresa Cullen, Pima County’s health director, said in a separate news conference.
Arizona on Tuesday reported more than 3,000 additional confirmed COVID-19 cases and 120 more deaths. The case number was an undercount due to a reporting issue with one provider, according to the state Department of Health Services.
Virus-related hospitalizations continue to climb, with 2,551 COVID-19 patients occupying inpatient rooms as of Monday. That’s about half the number of virus hospitalizations during the peak of last winter’s surge, but currently, there is little available capacity statewide because many hospitals are also caring for large numbers of non-COVID patients.
Arizona’s seven-day rolling average of daily new cases in Arizona was just under 4,000 as of Sunday, up from just over 3,000 two weeks earlier, according to Johns Hopkins University data. Meanwhile, the rolling average of daily deaths rose from 36.3 to 41.3 during the same period.
A rubber band can be stretched only so far before it snaps, said Dr. Keith Frey, chief physician executive for Dignity Health.
“We’re very close to that point,” Frey said. “Exhausted nurses. Exhausted doctors. Please help us help you.”
Republished with the permission of the Associated Press.