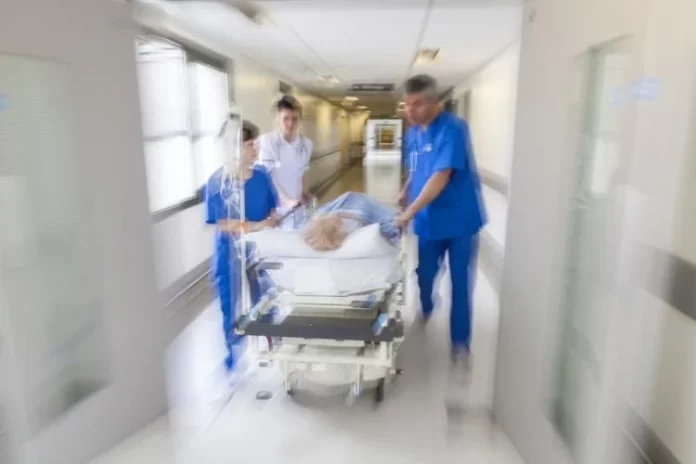
Nonprofit hospitals are among the most important safety net institutions in the United States. Thousands of times each day, they treat low-income patients without insurance at no cost to the patient. In 1992, in order to support this charity work, the federal government created the 340B drug discount program for nonprofit hospitals and clinics.
The 340B program allows these nonprofits to buy drugs at very steep discounts compared with other customers, providing substantial revenues for the bottom lines of hospitals. Consider an example of how this program boosts hospitals’ revenue. Suppose a hospital could purchase an oncology drug for $25,000, a 75% discount from the drug’s market price (and a discount level not uncommon in the 340B program). However, if the hospital dispensed that drug to a patient with good insurance coverage, they may be able to bill that insurance company at $100,000, allowing the hospital to pocket a profit of $75,000 on a single prescription.
One economist recently concluded that the 340B program had boosted nonprofit hospital revenues by $40 billion in a single year, 2019. When they created the 340B program, Congress thought that this additional revenue should be devoted to charity care programs. Unfortunately, at many nonprofit hospitals, charity care has been declining at the same time that revenue from the 340B program have been exploding.
A recent Wall Street Journal analysis concluded that nonprofit hospitals that secure billions through the 340B program provide less charity care than for-profit hospitals that receive zero revenue from the 340B program. “These charitable organizations, which comprise the majority of hospitals in the U.S., wrote off in aggregate 2.3% of their patient revenue on financial aid for patients’ medical bills,” write Anna Wilde Mathews, Tom McGinty, and Melanie Evans in an investigative report for the Wall Street Journal. “Their for-profit competitors … wrote off 3.4%, the Journal found in an analysis of the most recent annual reports hospitals file with the federal government.”
Louisiana’s Ochsner Health system drew special attention from the Journal for dedicating the skimpiest share of patient revenue to charity care, less than 1%.
Elsewhere, it was reported in February that Our Lady of the Lake and LCMC Health had committed a quarter of a billion dollars to Louisiana State University, the largest outside investment in university history. That’s all well and good until you realize that according to their June 2020-June 2021 Schedule H filing, Our Lady of the Lake contributes 0.5%, or $7.5 million – from a total of $1.54 billion – of its patient revenues to charity care. Did the hospital’s 340B funds pay for a huge investment in LSU’s research?
It is true that many nonprofit hospitals have challenges with low reimbursements from the Medicaid program, labor shortages, and other difficulties. Therefore, Congress could do one simple thing that may improve the 340B program and increase patient access to charity care: transparency.
Congress should require nonprofit hospitals and clinics to publicly report the amount of revenue that they are securing through the 340B program, and they also should be required to report, under a uniform definition of charity care, the level of free or discounted care they are providing. That way, policymakers could see if 340B revenues are largely being devoted to charity care, which was the intention of Congress, or if 340B funds are being diverted to executive compensation, hospital acquisitions, or other expenses.
Sadly, many nonprofit hospitals have lost their way and have gotten away from the mission that animated their creation: helping those in dire economic need afford healthcare. That needs to change.
William S. Smith, Ph.D., is a Senior Fellow and Director of the Life Sciences Initiative at Pioneer Institute in Boston.